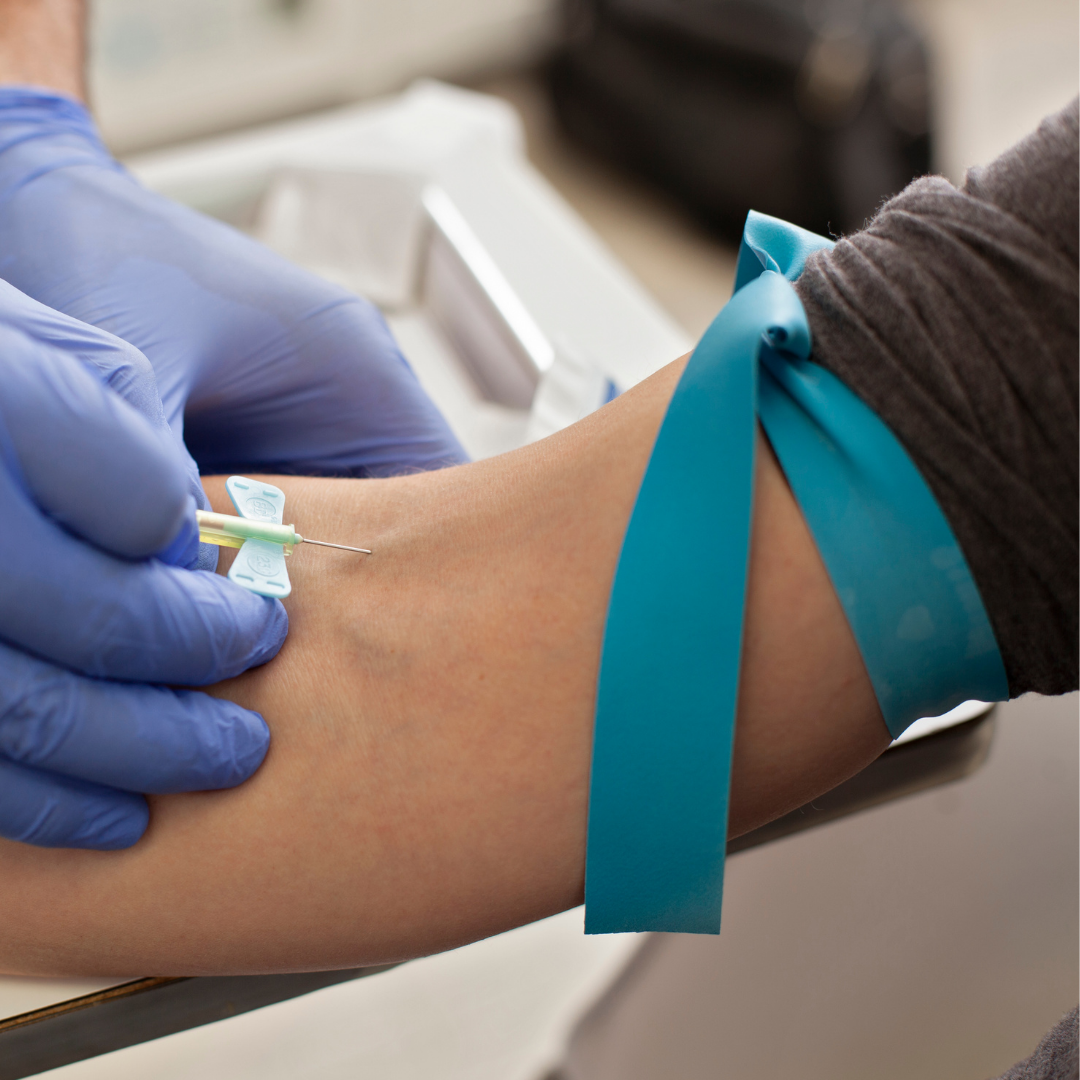
What Blood Tests Do I Need in Perimenopause?
Blood tests for hormones are notoriously unhelpful when used to make a diagnosis of perimenopause. This is because the perimenopause is a time of hormonal fluctuations. It’s often not until very close to, or sometimes even after periods have stopped, that changes show reliably on blood tests. The diagnosis of perimenopause is therefore a clinical one based on symptoms.
Do I need blood tests to diagnose perimenopause or menopause?
In the UK, NICE guidelines for the diagnosis and management of menopause state that in women aged 45 years and over, blood tests for hormones such as Follicle Stimulating Hormone (FSH), oestradiol and progesterone aren’t required in an otherwise healthy woman who has symptoms fitting with menopause, or whose periods have changed.
In women under the age of 45 years, hormonal bloods tests can sometimes be helpful if periods have changed, or to exclude other possible causes for similar symptoms. However, a normal range hormone blood screen does not exclude the symptoms being because of perimenopause, especially if there isn’t another explanation for the symptoms being experienced.

Do I need blood tests to start HRT?
For women who are 45 years or over, NICE guidelines state that where symptoms are fitting with menopause or perimenopause, then blood tests are not required before starting Hormone Replacement Therapy (HRT). This is because it’s very common for women in this age group to be experiencing menopausal symptoms, and there’s no additional value in performing the tests. In fact, in some cases, they can even add confusion.
For women under the age of 45 years, where another diagnosis for the symptoms isn’t strongly suspected, some doctors, particularly specialists with experience in managing menopause, are happy to prescribe HRT without blood tests. However, many doctors may also request a routine wellbeing blood screen. These bloods might include hormone tests, and usually a screen for other causes of similar symptoms, for example to check for thyroid problems, anaemia, B12 or folic acid deficiency, or for type 2 diabetes.
It’s important to be aware however, that a ‘normal’ range hormone blood test doesn’t mean that a trial of HRT might not be helpful if a more serious cause to explain the symptoms hasn’t been found. This can still be perimenopause.
When might blood tests be useful?
There are several reasons why blood tests can be helpful in supporting the care of women in midlife. For younger women, under the age of 40 years, it would be important to have blood tests when trying to make a diagnosis of Primary Ovarian Insufficiency (POI) or early menopause.
For older women, FSH blood tests can be used when deciding whether or not contraception is still required. The Faculty of Sexual and Reproductive Healthcare (FRSH), part of the Royal College of Obstetricians and Gynaecologists, have guidelines doctors use when helping with this advice; we know that blood tests can’t be relied on when already taking the combined contraceptive pill or HRT.
Many specialists or GPs experienced in prescribing HRT use hormone levels of oestradiol to both guide their prescribing, especially at higher doses, and also to check that transdermal products e.g. patches, sprays or gels are being effectively absorbed.
Finally, blood tests are used when considering the addition of testosterone and also monitoring it’s safe dosing and prescribing in the longer term. The results are used to calculate Free Androgen Index (FAI), a measure of the proportion of testosterone in circulation which is available to the body’s cells.
What level of oestrogen is normal on HRT?
Routinely there is no guidance stating that oestradiol levels should be checked while a woman is taking HRT. This is because the dose of HRT is based on the improvement or otherwise of symptoms. When oestradiol levels are checked, most often in specialist clinics, they can help to guide dosing, but there is no definite level which doctors would call ‘correct’.
The reason for this is that the levels of oestrogen required to improve symptoms, while also protecting the bones, varies depending on a woman’s age and stage of menopause.
Levels of oestradiol can also vary wildly during the perimenopause. Younger women with POI may need much higher levels, while post menopausal, and older women may be better with much lower levels. This is the reason that individualised care, rather than a one size fits all approach, is so important.
In summary
Perimenopause and menopause should be symptom assessed in the vast majority of women, other underlying medical conditions and clinical considerations notwithstanding. Normal blood levels are no reason to refuse HRT if a woman wants to try it as fluctuating hormones more often than not make results unreliable.
Dr Liz Andrew has worked as a GP for over 12 years and has developed a passion for offering women menopause care. She is an advocate for giving women the knowledge and support they need to make choices about their own bodies at a time in their lives that can feel fraught. She understands the unique and often misunderstood pressures on women which can become particularly difficult during the hormonal changes of peri menopause and thereon. She prescribes body identical HRT and encourages the use of lifestyle adjustments to actively improve wellbeing.
Dr Liz Andrew is part of the team of Menopause Specialist GPs at https://menopausecare.co.uk/
www.harleystathome.com | Instagram @harleystreetathomemenopause
Facebook: Search Harley Street at Home: Diagnosis, Symptoms & Treatments or Harley St at Home: Lifestyle, Self-Care and Lifestyle to join our private community